
Audio By Carbonatix
When the new coronavirus started to make headlines earlier this year, Olivia Boeck and her family did what many others did: They bought supplies, went to the grocery store once a week, and worried.
Boeck is a 29-year-old stay-at-home mom, raising a 2-year-old and 5-year-old with her husband in Gilbert. Her husband works for a company that installs radiology equipment. Every day, he goes in and out of hospitals.
Over the weekend of March 21, her husband came down with a sore throat. Soon, he was coughing. The following Monday, he called in sick to work, and Boeck took care of him. She called an urgent care clinic run by Dignity Health, which directed her to the Arizona Department of Health Services, which told her to try Banner Health’s drive-thru testing. Banner representatives, almost miraculously given the dearth of testing in Arizona, told Boeck that her husband met the criteria to get tested.
He went in that very day. The results would come in five to seven days, Banner said.
The next day, Tuesday, Boeck started to feel fatigue, one of the symptoms of COVID-19. But for her, getting tested would prove impossible.
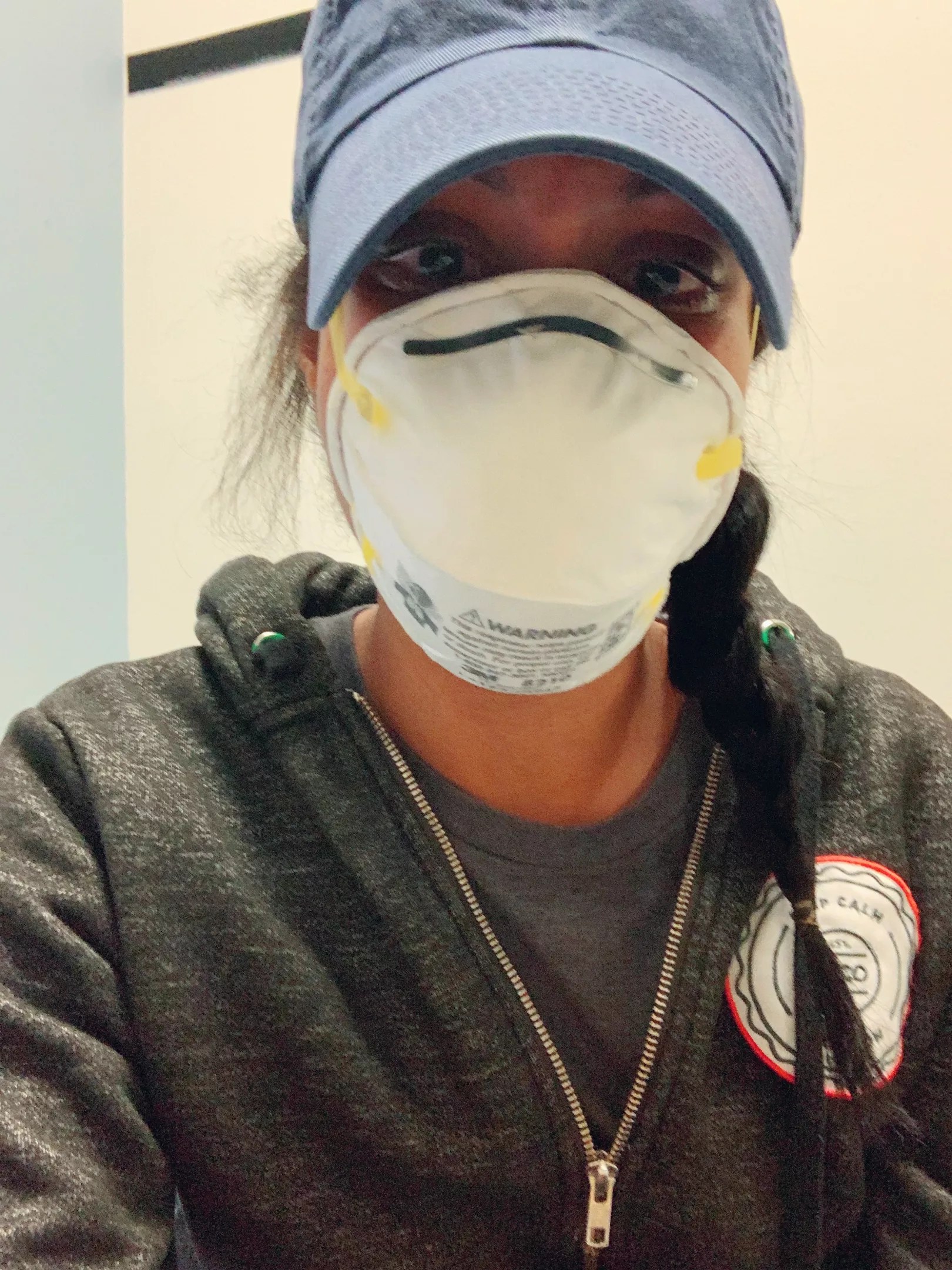
Olivia Boeck in the throes of her illness. She was denied testing for COVID-19.
Olivia Boeck
To date, Arizona has more than 1,200 cases of COVID-19, the illness caused by the new coronavirus. Twenty-four people have died. The state’s economy has seized, stopped in its tracks by calls for social distancing and formal restrictions closing bars and restaurants. On Monday, Governor Doug Ducey issued a stay-at-home order closing all services but those deemed, rather expansively, as “essential.”
In Arizona, as in many other states, the full scope of the virus’s spread is unknown. According to the state’s public health department, just 17,000 out of 7.2 million in Arizona have been tested so far. Reports abound in social media and in the news of people with serious symptoms denied testing who are told they don’t meet the strict criteria.
Last week, the director of the Arizona Department of Health Services, Dr. Cara Christ, told primary care providers to stop testing in order to conserve tests.
For patients like Boeck, the search for COVID-19 testing is an exhausting fool’s errand. For another Arizona woman, Kristan Landry, the quest for a test simply became absurd. Their ordeals show how ordinary people have been left to fend for themselves during a global pandemic of a deadly virus.
One physician for Banner Health, who spoke with Phoenix New Times on condition of anonymity out of fear of retaliation, feared that sick people who sought testing, whether they ultimately tested positive, negative, or were denied, were not getting the medical care they needed.
That doctor was one of several tasked with tracking the cases of patients who had been tested for COVID-19 at one particular testing site in Arizona. In five days, she said, there were six positives, 18 negatives, and 65 tests still pending.
One of the them involved an older man who had “abnormal X-rays,” she said. “He sounded like he was in a lot of distress.” His test results for COVID-19 hadn’t come back yet, and she feared that if they came back negative, the man – and his health – would be forgotten.
“At this point in time, there’s no process in place for making sure [people] get follow-up care if they’re not improving,” the doctor said.
‘What Testing?’
By Tuesday evening, Boeck was exhausted. She woke up the next day, Wednesday, with a fever and a sore throat. Swallowing gave her the sensation of drinking scalding coffee. When she tried to breathe, she felt as if her overweight cat was sitting on top of her chest. She wheezed just to catch a breath.
By midday, her temperature had reached 105 degrees Fahrenheit. She lay on the couch, weak and crumpled.

Olivia Boeck
Boeck called Banner, hoping to make an appointment at one of its drive-thru testing sites. But she was told that all appointments had been filled and Banner was out of tests.
Asked about that problem, Banner spokesperson Becky Armendariz said, “We have a certain number of appointments available each day at our drive-thru sites, and once those are booked we are unable to accommodate additional appointments.”
Boeck went to the emergency room of Mercy Gilbert Hospital, run by Dignity Health, because it was the hospital closest to her home.
When she arrived, the parking lot was empty save for two giant white tents, the kind Boeck associated with COVID-19 drive-thru testing. Outside of one sat a Gilbert police officer. She pulled up and asked him where the testing was.
“What testing?” the officer asked, as Boeck sat in her car, drenched in sweat and wearing a mask on her face.
There’s no testing at the tent, he told her, but she could go into the emergency room if she wanted. Desperate, Boeck walked through the doors. Behind a table sat a nurse, wearing no gloves and no mask, who did not take her temperature. As she signed in, Boeck was told it was fine for her to use communal pens.
A nurse walked her back through the emergency department to a triage room, where nothing but curtains separated her from everyone else. Through them, she could hear patients coughing and nurses whispering about reusing their masks, because “this is the only one you get.” At one point, someone at the hospital gave her a tissue for her to wipe her nose and her mouth, and told her to “just hang on to it.”
Guidance from the Centers for Disease Control and Prevention, or CDC, says that tissues should be thrown away as soon as they’re used.
By then, Boeck’s fever had dropped to 100 degrees Fahrenheit. Chest X-rays showed no pneumonia, and a flu test came back negative.
“And that was when the doctor came in and was just like, ‘Well, it’s possibly coronavirus, but we can’t test ya, so you can just go home and take Tylenol,'” Boeck told New Times.
Carmelle Malkovich, a spokesperson for Dignity Health, said its hospitals in Arizona were “not out of test kits.”
“Like everyone, however, the ability to test is still constrained across our community,” she added. “Therefore, our clinical teams are testing those most in need of our services per CDC guidelines.”
Two hours after arriving at Mercy Gilbert, Boeck was home.
By Thursday, her fever was “holding steady” at 103 degrees. Her body ached, still wracked by chills, and her husband was no better either, his cough steadily worsening. They cleaned obsessively and wore N95 masks – rotating through four of them, disinfected and reused – at home to try to protect their kids. Throughout all of their preparations for the new coronavirus, Boeck realized, they’d neglected to think about one essential thing.

Olivia Boeck and her husband, before they got sick.
Olivia Boeck
“We have masks, we have hand sanitizer, we have soap, we have all of the supplies we need, but we didn’t have a plan in place for what it would look like if one of us were to get sick,” she said. “That’s what people are forgetting.”
In the days that followed, Boeck’s blood pressure was too high. She lost weight. She went to a Banner urgent care center, and was again denied a COVID-19 test, despite being told that she looked “very sick.” All she was able to get were prescriptions for medications to help with her cough and her breathing.
“I don’t want to take a [COVID-19] test away from anyone who is sicker than me as I’m sure many are,” she texted New Times last week, as she lay isolated in her room, away from her children. “What I do need is some information as to whether or not this is like bronchitis and it will pass but I can be around my kids or if this is covid and I truly cannot be around my kids.”
“My kids are young,” she wrote. “They need me.”
On Tuesday, Boeck said that she was feeling better, although she still had a cough and little energy. She declined to discuss the results of her husband’s COVID-19 test.
“Overall, I’m disappointed by the health care system here,” she reflected. “We tout ourselves in being such an advanced country, but in the time of true crisis, we fail – lack of testing, proper supplies, and proper treatment for those that couldn’t be tested but clearly are very sick.”
A One-Month Ordeal
Kristan Landry finally got the results of her COVID-19 test on Monday, March 30, two months after she started having trouble breathing, her chest began to hurt, and a strange fatigue set in.
Her ordeal to get tested began on March 2, during a routine visit with her oncologist. Landry was diagnosed with breast cancer in 2005; it has since metastasized her to her lungs and brain, requiring a craniotomy that robbed her of her ability to speak, a condition known as aphasia.
Speaking and using the phone are hard for Landry – both to hear what’s being said and to respond. She can almost feel the delay in her head, as her brain processes what is happening, then sorts it out, all in slow motion.
Writing is easier. Emojis punctuate her texts. Sometimes, if she can’t find an interpreter to help her with phone calls to doctors, she gives up midway through.
Landry’s a single mother who grew up in the Valley. She suspended her career as a social worker to raise her kids, but was diagnosed with cancer when her elder child was just 5.
When Landry told her doctor in early March about the shooting pain in her left lung, he sent her next door, to the emergency room at Banner Desert Medical Center in Mesa.
There, providers ran a CT scan on her lungs and diagnosed her with pneumonia. As she lay in bed, she couldn’t help but notice the curtains that separated her from others, and how permeable they were. Landry went home with a prescription for an antibiotic, a reminder to call her primary care provider if her symptoms didn’t improve, and no COVID-19 test.
The antibiotic didn’t help. Landry, who also has asthma, still struggled to breathe. Simple chores, like doing the dishes, exhausted her, she told New Times via text message. But when she called her primary care provider, she was told to return to the emergency room. The doctor was “too busy” to see her.
On March 13, she went back to Banner Desert’s emergency room, where staff gave her a breathing treatment. It helped, a little. But Landry’s oncologist had told her she still needed to get tested for COVID-19 because she had an upcoming surgery related to her cancer that depended on the results.
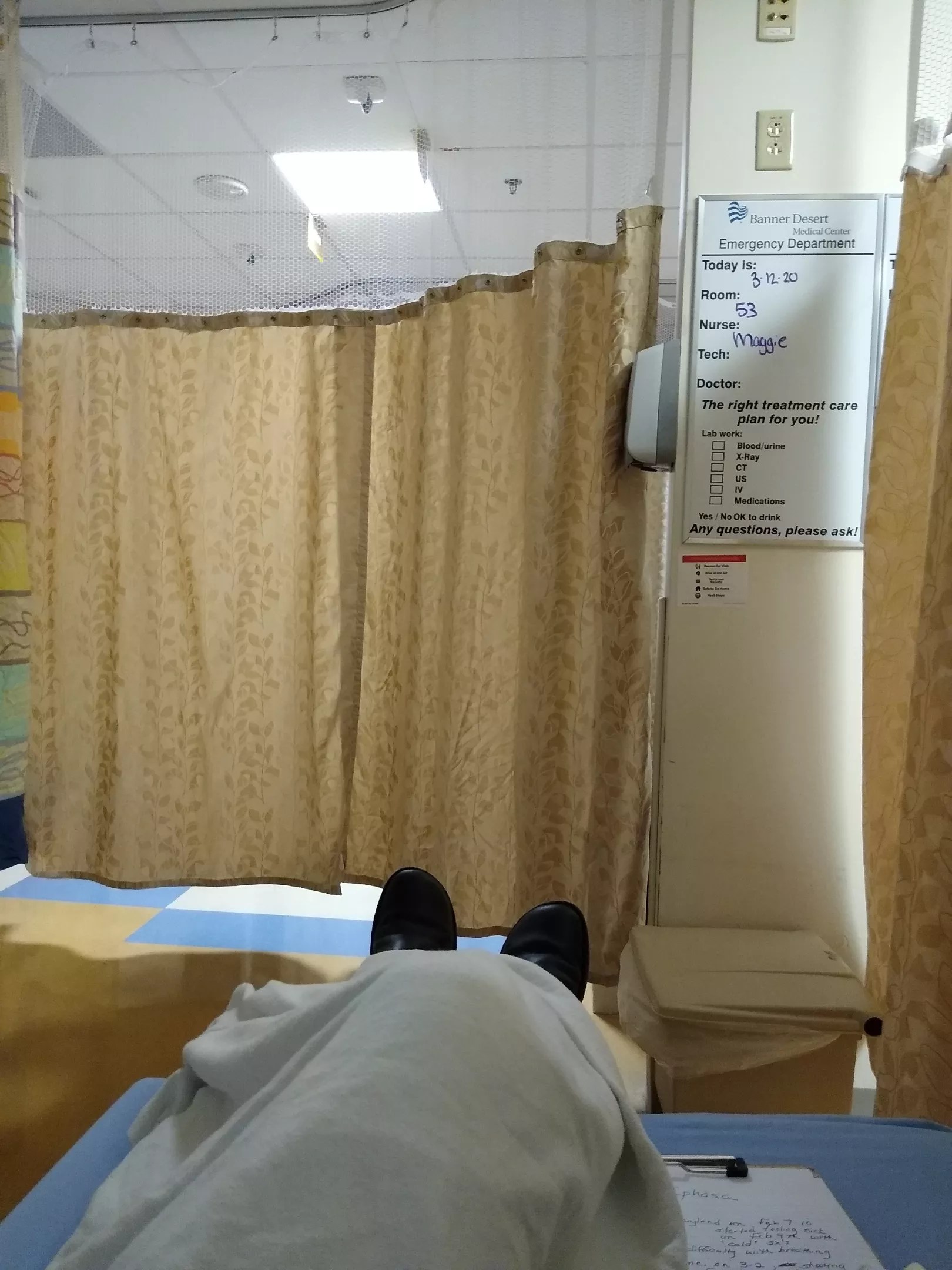
The view from a Banner Desert Medical Center emergency room bed on March 13.
Kristan Landry
She called her doctor again.
“Don’t worry about it,” the doctor said, when she asked about testing. The response felt condescending, even though she suspected the doctor intended it to be reassuring. She managed to schedule an appointment for an afternoon in mid-March.
Less than 24 hours before her appointment, the doctor’s office called. They would not see her in person, Landry was told. Instead, they would talk to her by phone.
Although the office denied it, Landry began to suspect that the doctor was refusing to see her because she had told them of her symptoms – something that primary care doctors have openly admitted they must do because they lack the equipment to protect themselves and other cases against potential COVID-19 cases.
But, she said, she was also told she needed to be seen by the doctor in order to get tested for COVID-19.
When she finally spoke with her doctor that afternoon in mid-March, the doctor said that primary care providers had been instructed not to order COVID-19 tests because the state didn’t have enough. Plus, she was told, she needed a fever to qualify for testing.
The next day, she woke up with a mild one.
The following week, as part of her cancer care, Landry had two appointments scheduled on back-to-back days, one for a bone scan and the other for a brain scan, at two separate Simon Medical Imaging labs in the east Valley.
On March 23, after the bone scan, the procedure left her feeling dizzy and struggling to breathe. She drove across the street to Dignity Health’s Mercy Gilbert Medical Center, to the emergency room, where she had blood tests and X-rays taken. Providers there told her she did not have pneumonia, and that they were out of COVID-19 tests.

Kristan Landry in the emergency room at Mercy Gilbert Medical Center on March 23.
Kristan Landry
The next day, Landry had the brain scan. But when she went in for the appointment – this one at a different Simon Medical Imaging lab, providers refused to see her until she got tested for COVID-19, citing her symptoms from the day before.
So, Landry went to the HonorHealth urgent care center next door to the imaging lab, where a physician’s assistant refused to read Landry’s handwritten notes of her symptoms, which she had put in writing because of her aphasia. Landry also said the physician’s assistant accused her of faking her symptoms.
Finally, Landry called 911 – from inside the exam room at the urgent care center – and landed, for the third time that month, in the emergency room of Banner Desert Medical Center. A sympathetic ER nurse intervened, and on Tuesday, March 24, Landry finally got tested for COVID-19. She was told the results would take two days.
The worst part of the ordeal, Landry said, was the trip to the HonorHealth clinic. She understood why doctors or the imaging lab couldn’t see her given her symptoms, but she vowed to never again return to any HonorHealth facility.
Six days later, Landry’s test result arrived.
It was negative, with a discomfiting caveat: “A negative test does not rule out the possibility of COVID-19 and should not be used as the sole basis of patient management decisions.”
Landry’s lungs still hurt. She is intensely fatigued, and if she pushes herself even slightly, she breaks into a cold sweat. She hopes to reschedule her brain scan soon.