
Google Maps

Audio By Carbonatix
A nursing assistant at a Prescott nursing home says she was told to continue to work with patients after informing her supervisor that she was symptomatic for COVID-19 – and also after she later tested positive for the disease.
Now, the state is investigating.
The facility, Granite Creek Health and Rehabilitation Center in Prescott, a skilled-nursing facility with more than 100 long-term residents and rehab patients from the local hospital, had been spared until early June from the pandemic. But as certified nursing assistant at the facility told Phoenix New Times, things spiraled out of control quickly after an employee tested positive for the novel coronavirus on June 9.
New Times is not disclosing the name of the worker based on her request for anonymity. Sick with COVID-19 and still trying to beat back the virus in home quarantine, she doesn’t want to return to Granite Creek and doesn’t want publicity.
“The state surveyor told me that they’re keeping my identity secret and calling me by the code name ‘Hero Worker’ LOL,” she wrote in an email on Tuesday. “I am still concerned that it being known that I reported this could affect my ability to find another job once I’m recovered.”
Mike Rasmussen, the facility’s administrator, confirmed on Tuesday that 16 staff members and 25 residents at Granite Creek have tested positive. He acknowledged in an email that the company would allow a COVID-positive staff member to come to work, and might ask but would not require that a sick staff member come to work.
The facility is owned by Ensign Services, a NASDAQ-listed company with nursing homes in several states. Barry Port, the company’s CEO, did not return a message.
As Granite Creek’s website shows, the 128-bed facility took some action in March when the pandemic hit, including the posting of “infection prevention” signs, “monitoring” staff and visitors for proper hand-washing and sanitizer use, and, “requiring staff to stay home from work if ill.”
The worker, a certified nursing assistant (CNA), told New Times that she has worked for Granite Creek for more than a year. CNAs typically work under supervision of a nurse, as they do at Granite Creek, but “we’re the ones who are right up close with residents,” she said. “We’re the ones helping them get up and out of bed… we’re the ones feeding them.”
The facility currently has 106 residents and/or patients, she said. Despite an employee testing positive on June 9, the facility didn’t step up its use of PPE (personal protective equipment) until June 17, when the staff was told that a resident in the long-term care hall had tested positive. Staff members then had to be be screened before entering patient-care areas, and started wearing face shields or goggles, and protective gowns more regularly, she said.
But then more patients began showing symptoms.
“From that point on, it spread like wildfire,” she said.
The facility converted a wing into an isolation hall full of patients waiting for tests to come back. When multiple tests came back positive, staff put up a “plastic wall” to separate the COVID-positive residents from those awaiting results.
Then multiple staff members began getting sick.
“I started feeling symptoms on June 20,” she said. That was a Saturday. The facility had nasal swabbing tests scheduled for staff members that Monday. She told the firm’s staffing scheduler that she was feeling sick, with symptoms including a headache.
“She said, ‘You are on the schedule until you hear otherwise,'” the CNA said.
She told her supervisor when she came in on Monday she was still feeling ill, and “she sent me to the floor to work. On Tuesday, same thing, they sent me out.”

Screenshots provided by New Times’ source.
Screenshot
On Wednesday, June 24, she called in sick. Her symptoms had worsened; she was now experiencing vomiting and diarrhea. Even after telling the scheduler about her symptoms, “she said I needed to be there.”
“I have diarrhea and I just threw up,” the CNA said in a text message screenshot she shared with New Times. “I’m sore everywhere, I feel like I got hit by a truck. I cannot work today.”
“I have you on the schedule for tonight,” replied “Tonya” from staffing.
“I’m still feeling really wiped out.”
“Get rest and I need you to be here.”
“At two?”
“Yes.”
The facility was experiencing a staffing shortage – because so many workers were out ill, the worker said. She was told to work the COVID hall, she said, which at that time had 18 patients, including eight who were confirmed positive. She didn’t report to work again. Another nurse who worked with her was also told she had to work, she said.
“On Friday, I woke up with no sense of taste or smell,” she said. “I went to urgent care. There were still no results form the work swab.”
She got another swab at urgent care and an order from a physician to stay home and self-quarantine. At 9:30 p.m. on Saturday, June 27, Rasmussen, the facility’s administrator, called her to let her know the swab at work had come back positive for COVID.
“He asked me if I’m symptomatic,” she said, and that Rasmussen told her if she was not, “they’ll have me work the COVID hall. I said I’ve been symptomatic all week. He said, ‘Let us know how you’re doing.'”
That night, she received another text message from the staffing scheduler.
“Mike called me last night and said my test for the day was positive,” she texted the scheduler. “I am still having symptoms and self quarantining.”
“You are scheduled to work and I have you on a positive all because you are positive.”
“I am still coughing, and I just vomited. I have a temperature of 99.1 with meds. I am not working sick.”
The worker said she wasn’t the only one who didn’t feel safe going to back to work, and she knows of other staff members who “are quitting or have quit.” At least three residents of the facility have died, and she knows of at least one Granite Creek nurse who was hospitalized with COVID symptoms, she said. Other employees she knew from the facility declined to call New Times with comments.
Rasmussen responded to questions with a lengthy statement that said it’s acceptable, based on Centers for Disease Control and Prevention guidelines, to put COVID-positive staff members to work with COVID patients.
All 25 residents who tested positive are still at Granite Creek, “cohorted and isolated away” from COVID-negative patients, and being cared for under CDC guidelines, he said in his statement.
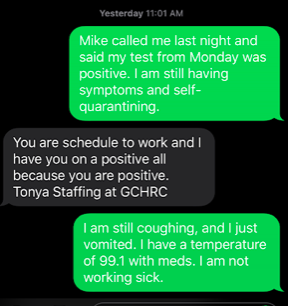
Screenshots provided by New Times’ source.
Screenshot
“Those staff members who have tested positive for the virus and are asymptomatic are appropriate to work with our COVID-19 positive residents – this assignment is also consistent with CDC guidance in such situations,” Rasmussen said. “Those staff members who have tested positive for the virus and are symptomatic are not working and not present in the facility. If an asymptomatic COVID-19 positive staff member indicates that he/she is not feeling well, they can certainly request to be off work. We would not ask a staff member who is ill, for whatever reason, to work with any of our residents regardless of COVID-19 status.”
“We communicate daily with the families and loved ones of our residents by phone, and we welcome their questions, calls or emails,” said in the statement, adding a word of thanks to his staff members.
Reminded in a follow-up email that the worker’s text messages indicated that the facility did ask a staff member with symptoms to come into work, Rasmussen replied: “Thanks for pointing out the discrepancy, and what I should have said is that we would not require [italics in original] a staff member to work in those circumstances. As indicated, it is acceptable for COVID-19 positive staff to work with COVID-19 positive residents – in such circumstances, we may ask employees who have tested positive to work on the COVID-19 unit and assist in providing care to the residents.”
CDC guidelines on health care workers with potential symptoms of COVID or a positive test seem clear on the federal agency’s web page, “Criteria for Return to Work for Healthcare Personnel with Suspected or Confirmed COVID-19 (Interim Guidance).” To sum up most of the guidance, it says such workers should be excluded from work. But scrolling down gets you to the emergency plan: “Healthcare facilities must be prepared for potential staffing shortages and have plans and processes in place to mitigate them, including considerations for permitting HCP to return to work without meeting all return to work criteria above.”
The CDC has a supplemental web page, “Strategies to Mitigate Healthcare Personnel Staffing Shortages,” that instructs health care facilities to come up with plans to allow COVID-positive staff to return to work under certain circumstances. Factors like whether the infected staff would work with immunocompromised patients would have to be considered, the CDC advises.
However, the state Department of Health Services isn’t advising facilities at this time to actually allow health care workers to work if they are symptomatic with possible COVID, much less COVID-positive: “If healthcare personnel develop symptoms consistent with COVID-19 (e.g., fever or respiratory symptoms), they must: Cease patient care activities. Put on a facemask immediately (if not already wearing). Notify their supervisor or occupational health services prior to leaving work.”
DHS spokesman Chris Minnick confirmed that state officials went to Granite Creek on June 30 “as part of a complaint investigation,” but said privacy regulations prevented him from releasing specific details.
In general, he said, the staff has been working with nursing home and assisted-living facilities to ensure they have proper safety guidelines in place to prevent COVID transmission.
Facilities do need to work on emergency plans to keep up care, but “our advice has been pretty consistent,” he said. “We absolutely want people who are sick to stay home to avoid spreading the disease – especially if they test positive.”
The novel coronavirus has marauded the country’s nursing homes and long-term care facilities in recent months, killing tens of thousands. A recent story in the New York Times states that 11 percent of cases and 43 percent of COVID deaths have occurred in nursing homes. In Arizona, the state DHS’ data dashboard shows that 601 “congregate setting” facilities have reported positive COVID cases, with the majority (204) being assisted-living centers.
The CNA said on Tuesday evening she was feeling better, but was still running a fever and had a cough.
“I’m not sure what will happen with the facility at this point,” she said. “I don’t intend to go back to work there.”