
Angela Spahr

Audio By Carbonatix
Like many Americans in April 2020, Angela Spahr was working remotely, from the safe and relatively mundane confines of her Scottsdale home.
But as she watched news reports of overwhelmed hospitals in New York, the 29-year-old medical device field specialist reasoned that she had the skills needed to fight the virus at its epicenter. Spahr had spent seven years working as a registered nurse in Banner hospitals across the Valley. So she enlisted in a special six-week COVID-19 response contract and traveled to New York.
“I just wanted to help out,” Spahr told Phoenix New Times recently, from the Brooklyn apartment she’s rented.
It was her day off. Hours before, she’d received a text from a co-worker: one of her patients had just died. Spahr recalled that, just days ago, the man was off his ventilator and seemed to be doing fine. “We did all that we could,” she said, “and it still wasn’t enough.”
It’s a turn of events Spahr has sadly become accustomed to. “I haven’t seen a lot of success stories,” she said.
Spahr said the hardest thing to see is people dying alone. Many of the patients she cares for are unconscious; nurses will hold up iPads so their family members can see them as they lay motionless and intubated, their chances for survival slim. “I’ve seen a lot of people pass away,” Spahr said. Many of them were in their 70s or older, but one was as young as 43.
In Phoenix, Spahr had worked exclusively in emergency rooms, where, she said, “we fix people.” When she arrived at New York Presbyterian Queens Hospital on April 20, she was assigned to work in the COVID intensive care unit. Over the course of her first four weeks of work in the ICU, she said she saw “maybe two or three” patients recover. Most of the people she treated there left only after they’d died.
Spahr learned on the job. Normally, a nurse would receive eight weeks of training before working in the ICU. But these were not normal circumstances. Spahr watched YouTube videos to learn the hospital’s charting system. “It was overwhelming,” she said. She compared the experience to working at a busy restaurant without proper training on the POS system. Except in Spahr’s situation, she wouldn’t just have an angry customer to deal with. A patient could die.
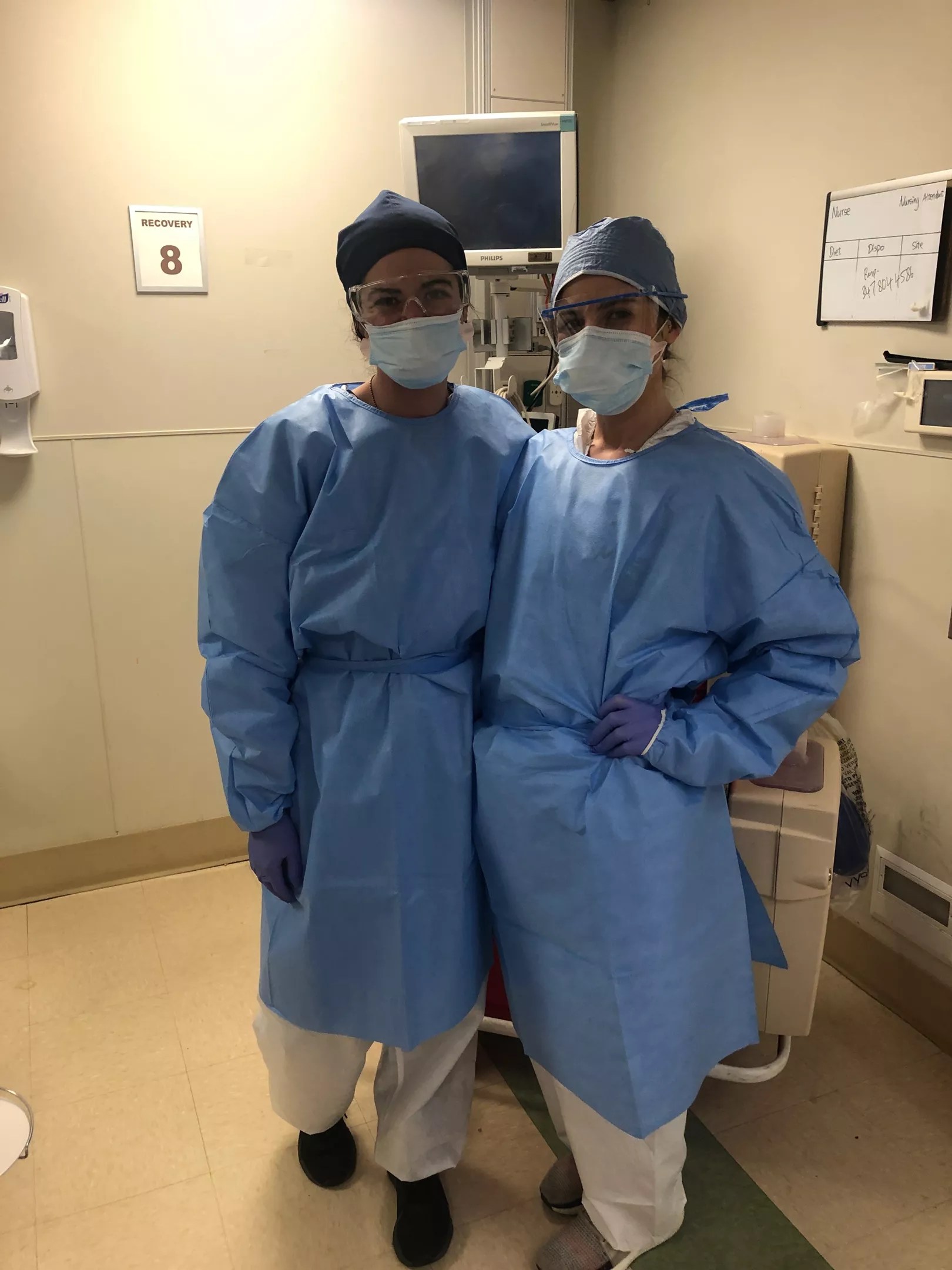
Spahr (left) and a fellow NYC nurse.
Angela Spahr
She said the typical capacity for the ICU space at the hospital was around 40 patients. On her first day, it held 99 patients.
“An astronomical number,” she said. “It was like walking into a war zone.”
Due to a lack of space, surgery recovery rooms and waiting spaces were converted into ICUs. Normally, ICU nurses work with one or two patients. But when Spahr arrived, each nurse was responsible for five or six. She said most of the COVID-19 patients there are on a complex cocktail of life-sustaining IVs, and it is part of the nurses’ job to ensure these medications are correctly calibrated – a task made exponentially more difficult the more patients you have.
“It creates an environment where it is easy to make mistakes,” she said. “If you were to just let one of [their IVs] run dry, some of them would die in a matter of minutes.”
As of June 1, there were over 6,200 COVID-19 deaths recorded in Queens. That’s about 6 percent of the U.S. death toll in a borough that represents just 0.6 percent of its population.
Beth Jacobs, an epidemiologist at the University of Arizona, says she thinks it is likely that New York City’s population density and high reliance on public transportation contributed to its deadly COVID-19 outbreak. While Arizona does not share those characteristics, she said she has “seen no convincing evidence that Arizona will not experience a great increase in cases within the next few months.”
If that happens, it is conceivable that the state could find itself short on ICU beds. As restrictions ease, and Arizonans head back to bars and the gym, Arizona Department of Health Services data shows that as of May 30, only 17 percent of the state’s ICU beds were available. On March 30, 31 percent were available.
“There is still so much we do not know about this pathogen,” Jacobs said. “I can only say with certainty that COVID-19 is not finished with Arizona yet.”
Despite the grim outcomes for the majority of her patients, Spahr is encouraged by the progress in the treatment of the virus she’s seen in the few weeks she’s been fighting it. Her hospital is now using the antiviral drug Remdesivir, which has been shown to speed recovery.
“They’re getting new research and data everyday,” she said. “We’re trying everything to save these people.”
Spahr’s biggest hope for her home state is that it avoids anything close to what she’s seen firsthand in New York. She said she has not experienced any symptoms of the virus, despite being exposed to it on a daily basis. She credits the efficacy of her PPE. When she gets back to Arizona, she plans to wear a mask.
During her time on the frontlines, she’s had a lot of friends back home ask if it’s “really as bad as they say it is.” The question, she said, is offensive.
“Yes,” she replies, “It’s so real. I wish you could see how sick these people are.”