
New Times iIllustration

Audio By Carbonatix

New Times iIllustration
No one saw Emelynn go under.
Her older siblings, just a few feet away, splashed in their family’s pool in Buckeye. Her babysitter, distracted, played with another toddler. Her dad left the grill to fix a loose screw on the trampoline. Her mom was in the checkout line at the store, four miles away.
At least 20 adults were at her mother’s birthday party on June 10, and yet no one saw 18-month-old Emelynn Davis go under. There she was, free-falling without floaties into the 3-foot-deep water.
One minute passed, and water entered her throat and blocked her airway.
Two minutes passed, and oxygen stopped flowing into her bloodstream.
Three minutes, and she lost consciousness.
Four minutes — oxygen stopped reaching her brain.
Five minutes — her throat relaxed and water rushed into her lungs.
It wasn’t until one of the older kids got out of the pool that they noticed Emelynn face-down in the shallow end.
That evening, Emelynn almost became one of Maricopa and Pinal County’s 56 residents who died from drowning this year.
Of those deaths, 14 were children under 5, according to The Drowning Prevention Coalition of Arizona. An estimated 390 children die due to drowning each year in the U.S.
Despite longstanding prevention efforts, drowning continues to be one of the leading causes of death and injury in children, making the headlines that follow just as common.
News alerts of children drowning become white noise in a state like Arizona, where the frequency is 25 percent higher than the rest of the country.
Often, stories are divided into heroic first responders or mourning families. The lesser-known stories are those of the struggle to recover — the story of Dorothy and Russell Davis and their baby Emelynn.
There are small victories and large sacrifices for survivors and families.
The Davises aren’t looking for a small victory. They’re looking for a miracle that will help them all heal.
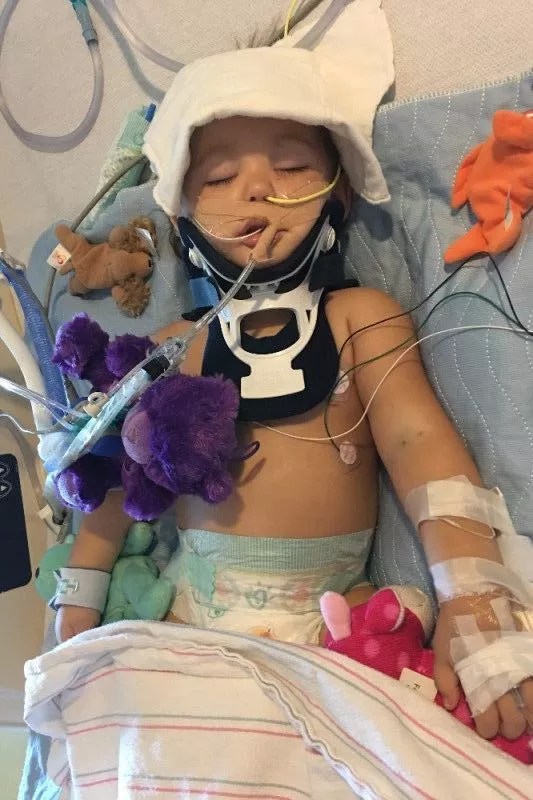
Emelynn spent seven weeks at Phoenix Children
Courtesy of Dorothy Davis
Dorothy Davis was not supposed to host her 37th birthday party.
There were not supposed to be 12 bags of ice melting in the 102-degree sun. There was not supposed to be barbecue chicken on the grill. There were not supposed to be 10 kids in the pool.
Dorothy told her fellow biker friends that she refused to organize her own party, but they weren’t willing to let her off that easy. The plan was to meet at the New Founders of Freedom Bike Shop 1 in Avondale for cake after a small gathering for dinner at a friend’s house.
Then the shop’s air conditioner and drink cooler broke.
So everyone headed to the Davises’ five-bedroom home at the back of the cul-de-sac in the WestPark neighborhood of Buckeye. And Dorothy headed to Walmart to buy extra chips and pop.
This kind of day had played out dozens of times in the Davis’ backyard, which was often a constant flurry of activity.
But June 10 turned out differently.
The pool didn’t have a fence, so the Davises created safeguards for their baby girl. She wasn’t allowed to run out to the backyard without an adult. Whoever opened the self-locking door for her was on baby duty.
But in that moment, when Emelynn stepped out of her pink, inflatable kiddie pool and into the big pool, no one was on baby duty.
When they pulled her out, Russell was the first to attempt CPR. He knew all the moves from his junior lifeguard days as a boy, but as he leaned over Emelynn’s limp body, his mind went blank.
His youngest daughter was turning blue.
Friends with CPR training, Brian Christian and Katelin Steinke, stepped in. Inside, someone called 911. Another friend gathered the kids and brought them to a neighbor’s house.
Foam started coming out of Emelynn’s eyes, nose, and mouth. Russell reminded them to turn her head to let any liquid out.
She didn’t have a pulse.
Dorothy was next in the Walmart checkout line when her friend got the call.
“What do you mean she fell in? Is she okay?”
Dorothy feared immediately it was her youngest, Emelynn. She prodded her friend with questions — did she bump her head? Was she bleeding?
Her friend’s eyes widened.
“The paramedics are working on her.”
They left everything in the cart and sprinted to the door. From the passenger seat, Dorothy shouted to go faster as they drove down I-10 East.
When she arrived paramedics had started a third round of CPR.
Finally, Emelynn spit up water and took a breath.
She thrashed around so violently first responders induced her with ketamine, propofol, and morphine — a cocktail that could knock out a grown man.
Her blue eyes fell into a dreamy slumber as she was rolled out on a stretcher.
Emelynn was airlifted to Phoenix Children’s Hospital — a 40-minute drive from home. The cul-de-sac was lined with emergency vehicles, so the helicopter was forced to land in a park down the street. Emelynn was wheeled into an ambulance to bring her the 500 feet to the park.
Dorothy and Russell grabbed a phone charger, got in the first car that wasn’t blocked in, and tore out of the neighborhood. They beat the chopper to the hospital by two minutes.
Dorothy expected the worst as she and Russell stood in the 2-by-6-foot yellow box painted as a boundary for parents in the doorway of the trauma room.
Doctors stabilized and sedated the little girl once more for an MRI.
Dorothy pleaded with God to let Emelynn survive and live a normal life.
Nurses wheeled Emelynn through the colorful hallways of Phoenix Children’s Hospital. Yellow, orange, and green walls passed by until they turned into the intensive care unit.
She had so many tubes and wires coming out of her that she looked like a cable box.
A yellow one in her nose, one clear tube, and one thin white wire looped into her mouth. Three different IVs went in and out of her left arm. A neck brace kept her head still.

Dorothy Davis researched alternative medicine and therapy practices for Emelynn after doctors said her daughter would never walk again.
Jim Louvau
Her initial scan showed no brain damage, but her mother knew better. She knew it could take up to 72 hours for brain damage to register.
Brain damage normally occurs after just five minutes without oxygen. One-third of drowning survivors sustain long-term brain damage and disability. There is little hope in the medical community of a full or even substantial recovery after a drowning.
One study even went as far to say survivors “will consequently be a great burden to their family and society for the rest of their lives.”
Dorothy is a realist. Her background as a medical coder for insurance companies gives her a no-bullshit attitude when it comes to medical jargon.
She asked doctors to give it to her straight. She wanted to know exactly what her daughter’s recovery would look like.
When Emelynn’s second scan came back with moderate brain damage, doctors told Dorothy Emelynn would be on a combination of seizure medications from here on out, she would have little interaction with the world around her, and she would live her life with eyes glazed over.
For the next 48 hours, Dorothy cursed God in her head. Why let her baby girl, still six months shy of her second birthday, survive this if she would be bound to a life of ventilators, feeding tubes, and wheelchairs?
Why not show mercy and take her?
Why make her suffer?
Dorothy knew she couldn’t wave a magic wand and bring Emelynn back to that smiley baby she was just a few days before, but she had to do something.
She told herself: “Expect the worst. Let yourself believe maybe this will be your truth from here on out, but don’t ever say, ‘This is my truth from here on out.”
Within the first 10 days in the hospital, she found support groups on Facebook, she researched different types of therapies, and she set up meetings about special education to know what to expect when Emelynn was in school.
Then she discovered HBOT.

During a Hyperbaric Oxygen Therapy (HBOT) session the patient sits in a chamber where the pressure is lowered to below-sea-level.
Lindsay Moore
Hyperbaric oxygen therapy, HBOT, is an alternative treatment that is believed to enhance the body’s natural healing abilities by inhaling pure oxygen.
Much like scuba diving, hyperbaric “dives” happen at below- sea-level pressure. By dropping the pressure in the HBOT chamber, oxygen molecules are squeezed small enough to dissolve deeper into the skin and flow into red blood cells and blood plasma.
The idea is to help facilitate oxygen flow to hard-to-reach spots, like wounds on the brain, and to heal inflamed tissue and boost cells.
A family member forwarded Dorothy a news clip of a 2-year-old from Arkansas who was being called a miracle after being underwater for at least 10 minutes.
Eden Carlson had pushed through her baby gate and fallen into her pool in February 2016. Just like Emelynn, doctors predicted Eden would never walk, talk, or even eat on her own.
Unwilling to accept such a dismal fate for their daughter, the Carlson family turned to Dr. Paul Harch, clinical professor and director of hyperbaric medicine at Louisiana State University Health New Orleans School of Medicine.
When Eden made progress — laughing, talking, even climbing up stairs — her story made national news. She was the toddler whose brain damage “reversed,” something the medical community had never seen before.
Dorothy read Eden’s story and messaged her mother, Kristal Carlson, on Facebook. Dorothy asked Carlson specific questions, like how long Eden went without oxygen, what temperature was the water, and how many minutes paramedics performed CPR.
Eden’s accident seemed worse than Emelynn’s, making her progress all the more remarkable.
Carlson wouldn’t make Dorothy any promises. She told Dorothy she could never predict what would work for Emelynn, but she knew HBOT worked for Eden.
HBOT therapy sessions usually cost upward of $100 for each hour, with most patients seeing significant results after 40 dives. It’s a lot of money to spend on uncertainty.
The FDA has approved HBOT for 14 different health conditions ranging from carbon monoxide poisoning to thermal burns.
Anoxic brain injury, when the brain lacks oxygen, has not yet made the approved list, although is it being studied. In short, this means insurance doesn’t cover HBOT therapy for drowning victims.
Although the treatment claims to have origins dating back to the 17th century, it is still not common practice in the United States. Many medical professionals consider it to be more of a money-suck than a reliable treatment program.
Serenity HBOT owner Rick Ryder thinks they’re just nonbelievers.
Ryder started researching HBOT after doctors couldn’t figure out why his daughter wasn’t growing properly; they would later reach a diagnosis of Addison’s disease.
What started in his garage as a passion project manufacturing HBOT chambers grew into a successful small business in 2006. Now, Ryder’s distributor ships out about 20 chambers a year to HBOT facilities worldwide — including Harch’s center in Louisiana.
Ryder also has a therapy business in Glendale, which treats an average of 65 patients a week who sit in any of the four chambers hoping to solve a variety of health issues from stroke recovery to autism.
Family members helped Dorothy research local HBOT facilities to ask about prices and treatment plans. It was more than just a good deal that drew Dorothy to Serenity, though; it was the kindness the staff showed her.
“Every question we’ve had, the answer is ‘We’re going to help you,’’’ she said.
Each session at Serenity costs the Davises $80 (a discounted price for purchasing 40 sessions). Although it’s less than half what Harch charges at LSU, the cost of HBOT was still out of reach for the Davis family.
Luckily, they had a group of tattooed, leather-jacket-wearing, Harley Davidson-riding guardian angels to swoop in and help.

Emelynn started HBOT sessions just two days after she left Phoenix Children’s Hospital.
Lindsay Moore
Dorothy and Russell’s charitable fraternal order, The New Founders of Freedom, is a close-knit group of almost 100 bikers, which serves veterans in the community.
Their symbol is a bald eagle with two rifles crossed, shooting out American flags — the American patriot version of skull and crossbones.
This rough and tough group has a soft spot for Little Tank — Emelynn’s road name. They’ve raised more than $5,000 for Emelynn’s therapies and even chipped in for the Davises rent a couple of times.
Dorothy and Emelynn began the HBOT treatment just two days after Emelynn was out of the hospital. They sat across from each other among gymnastics mats and pillows set up in the 6-foot by 11-foot cylinder for their first session.
The pill-shaped fortress was dark with the humming of oxygen tanks outside the quarter-inch thick wall.
Doctors shrug their shoulders at the alternative therapy. HBOT won’t hurt, but they can’t guarantee it will help. There’s just not enough evidence to prove that repaired brain tissue is a result of HBOT and not just the body’s natural healing habits at work.
After seven weeks in the children’s hospital, Emelynn blew through everyone’s expectations. She smiled, giggled, and was just as curious as most kids her age.
There were physical signs of her accident still. Sitting in the chamber, Emelynn mirrored a baby who was just learning to use its body, often flailing for balance. When she sat up it was all at once, like a strong breeze blew through and propped her up. Her body swayed a little before she collapsed forward with the same uncontrollable momentum.
Emelynn hinged at the waist like a marionette, and her mom and ever-present puppeteer, was there to tug the strings and prop her back up to play games and watch Minions on her iPad.
The inside of the robin’s-egg-blue submarine felt like it was sinking 15 feet below sea level. Emelynn was too young to hook up to an oxygen tank, which would normally push 100 percent medical-grade oxygen through her little nose.
Emelynn and her mom sat in the chamber for an hour while the pressure rejuvenated what was lost, repaired dormant brain tissue, and allowed for the creation of new neurological pathways.
Their ears popped, and Emelynn’s brain started to heal. Dorothy was right there, healing with her, one hyperbaric dive at a time.

The Davis family is healing together after the youngest daughter, Emelynn, drowned in June.
Jim Louvau
By August, the Davises started to fall into a routine. The older kids went back to school and a 5-foot by 7-foot calendar created with electrical tape dictated Emelynn’s schedule. The color-coded grid of appointments, locations, and times covered nearly the entire wall in the front hallway.
Monday through Saturday, the schedule showed a new arrangement of five different therapies with doctor visits peppered in.
They crisscrossed the Phoenix area: 9 a.m. eye doctor, 2 p.m. HBOT, 5 p.m. speech therapy.
Russell fell into the false sense of normalcy and expected Emelynn to make a full recovery. Dorothy reminded him that this new life — a Sudoku puzzle of appointments, medicines, and therapies — might be their reality forever.
Emelynn was no longer the independent little girl she once was. She followed her mother around the house 24/7. She didn’t entertain herself while Mom worked or hold Mom’s hand when they walked into a store.
Emelynn needed to be carried, comforted, and constantly monitored.
The world had changed for Emelynn, but Mom stayed the same.
For Dorothy, it was déjà vu. She had a newborn all over again.
There was a list of firsts that were familiar: rolling over, sitting up, and smiling.
And firsts that were new: meeting a water intake goal or a full day without the ventilator.
“It’s heartbreaking at the same as it’s joyful,” Dorothy said. “I knew who she was before.”
Emelynn started crawling, laughing, and smiling — actions doctors never expected her to do. But she used to run, dance, and play with her siblings.

Emelynn no longer takes any seizure medicines and is on a more natural regimen of CBD oil and melatonin.
Zack Allard
With every new milestone, there was the remembrance of how Emelynn was before.
The whole family was left to grieve for someone who was still with them.
Dorothy calls this her deepest, darkest circle of hell. Often, she felt it was so deep not even Russell could tread there with her; only her mother, Dwlinda, was there to hold her hand.
It’s hard not to place blame or get angry over what was taken away from her baby, Dorothy said. There are days when her patience wears thin and she wants to scream at her husband: “You’re the reason Baby is broken.”
But words can’t be unheard, so those aren’t the words she says. Instead, she reminds herself of the ever-expanding support system she’s gained. She reminds herself that this was an accident. That Russell is a good father.
She knows Russell would never do anything to hurt Emelynn or her four siblings: 8-year-old Dezlynn, 12-year-old Killian, 13-year-old Malachi, and 13-year-old Chase.
The kids had questions about Emelynn’s accident and her recovery: Would she be like the other kids they saw at school — the ones who rode a different bus and had a special classroom?
Most likely, yes. She will learn more slowly than most kids her age. Because Emelynn was so young, her moderate brain damage meant months of development were lost in a short amount of time.
In kid language, Emelynn is not 100 percent better. She may never be. But, if she can get to 80 percent, well, that’s a B.
Would the damage in her brain get worse? the kids asked.
No, what’s done is done. There is only moving forward.
After a few weeks of being home, Emelynn started her favorite game of stealing shoes. She brought her brother’s shoe over to her mom on the couch; Dorothy repeated, “that is a shoe,” trying to generate a response from the baby she was told by doctors would only ever respond to the simplest of commands.
Then Emelynn lifted up her foot. She understood. She was still in there.
In that moment, Dorothy had hope.

Emelynn Davis receives physical, occupational, and speech therapy at Phoenix Children’s Hospital.
Zack Allard
In October 2016, Dorothy was recording Emelynn taking her first steps at 10 months old.
One year later, in the east building of the children’s hospital, they were working toward the same milestone.
Emelynn locked her legs when she stood and tried to walk. Her occupational therapist, Alex King, was right behind her, correcting her form. She passed by the red and yellow mesh tunnel she just crawled through and was working her way around the room. She looked like she was on stilts as she headed toward a big, red exercise ball.
King lifted her up and let her get in a few bounces before he put her back to work.
He positioned Emelynn into a lunge-like kneeling position, one of her current goals. Instead, she hyper-extended up out of it and into a Frankenstein standing position.
King knocked her back down to her knees. Emelynn turned around with a look of disapproval in her big blue eyes.
“I’m sorry,” he said to her. “You’re doing it wrong.”

Doctors expected Emelynn to be wheelchair bound for the rest of her life, but she proved them wrong.
Zack Allard
For the first three weeks after her accident, Emelynn was blind. Even though her eyes were not damaged, her brain couldn’t make sense of what they were seeing. King used wooden blocks to help reteach Emelynn how to identify shapes and colors.
Sorting toys only held Emelynn’s attention for a few minutes. She was more interested in climbing the miniature staircase in the center of the room — a task that was a step ahead of King’s plan, as always.
“She met my short-term and long-term goals before my short-term goals were due,” King said.
King attributed Emelynn’s success to a combination of factors: the immediate CPR, the paramedic’s four-minute response time, and the airlift to Phoenix Children’s Hospital. The largest factor, though, is the Davis family’s commitment.
“Momma is her biggest motivator,” King said.
Emelynn was clutching her mom’s iPhone as she plopped down on the last step.
“Take it to Momma,” King said.
Emelynn took a few steps toward Dorothy, but stopped just short of her.
“Closer,” Dorothy said. “Come closer.”
This type of discipline is key to Emelynn’s development. At home, Dorothy was adamant in making Emelynn work for what she wanted. That was exactly what King wanted to hear.
“I could sit over there and she would run therapy,” King said of Dorothy.
After only nine weeks out of the hospital, Emelynn was no longer taking any seizure medicines. Instead, her daily regimen included a 100-milligram drop of CBD oil, a cannabis extract, twice a day and a small dosage of melatonin to help her sleep.
With her small army to help her, Dorothy spent endless hours talking with parents on forums and researching the alternative options they suggested.
“If somebody told us to roll her in goat poop and that would make her better, I would roll her in goat poop every day,” she said.
Not all of Emelynn’s doctors have appreciated Dorothy’s consistent line of educated questioning. Hyperbaric oxygen therapy and essential oils raise a lot of eyebrows in the medical community.
Emelynn’s physician at the hospital was quick to wave off what Dorothy called her “smelly oils” and other progressive therapy techniques.
“He just treated me like I was a quack because I had a lot of question about a lot of alternative medicines,” Dorothy said. “He just acted like Western medicine was the only thing out there.”
Phoenix Children’s Hospital does not have an official stance on alternative medicine, because it’s on a case-by-case basis. However, Dr. Angus Wilfong, associate director and chief of pediatric neurology, said he and his colleagues at the Barrow Neurological Institute at Phoenix Children’s Hospital are ecstatic about Emelynn’s progress.
Emelynn hasn’t had a seizure since her first week in the hospital, but Dorothy kept “rescue meds,” in her purse just in case. It’s not that she doesn’t trust Western medicine; she’s just quick to challenge the status quo.
“I don’t want her to be harmed in anyway, but I also don’t want her to have a giant cocktail of meds because she obviously doesn’t need them,” Dorothy said.

Emelynn went back in the pool with her parents after her accident.
Shawna Killgo
Emelynn’s second birthday was a little more than a week away when Dorothy sent out the Facebook event to the New Founders of Freedom in late November. The response was immediate — everyone wanted to see Little Tank.
Just six months after her accident, Emelynn was zig-zagging through the living room and kitchen at home in Buckeye while her sippy cup swung from her hand. She inspected the Christmas lights and porcelain snowy village laid out on the kitchen counter before she dashed back to the couch.
She lost momentum and crashed to the floor. But then, she picked herself up without assistance — her latest breakthrough.
She grounded herself in a wide stance with her feet turned out as if she was ready to drop into an exaggerated ballet plié at any moment.
As a Christmas gift, doctors plan to put ankle braces on Emelynn to help stabilize her and turn her feet in. The braces will take the place of occupational therapist King’s firm grip on Emelynn’s calves meant to correct her stance.
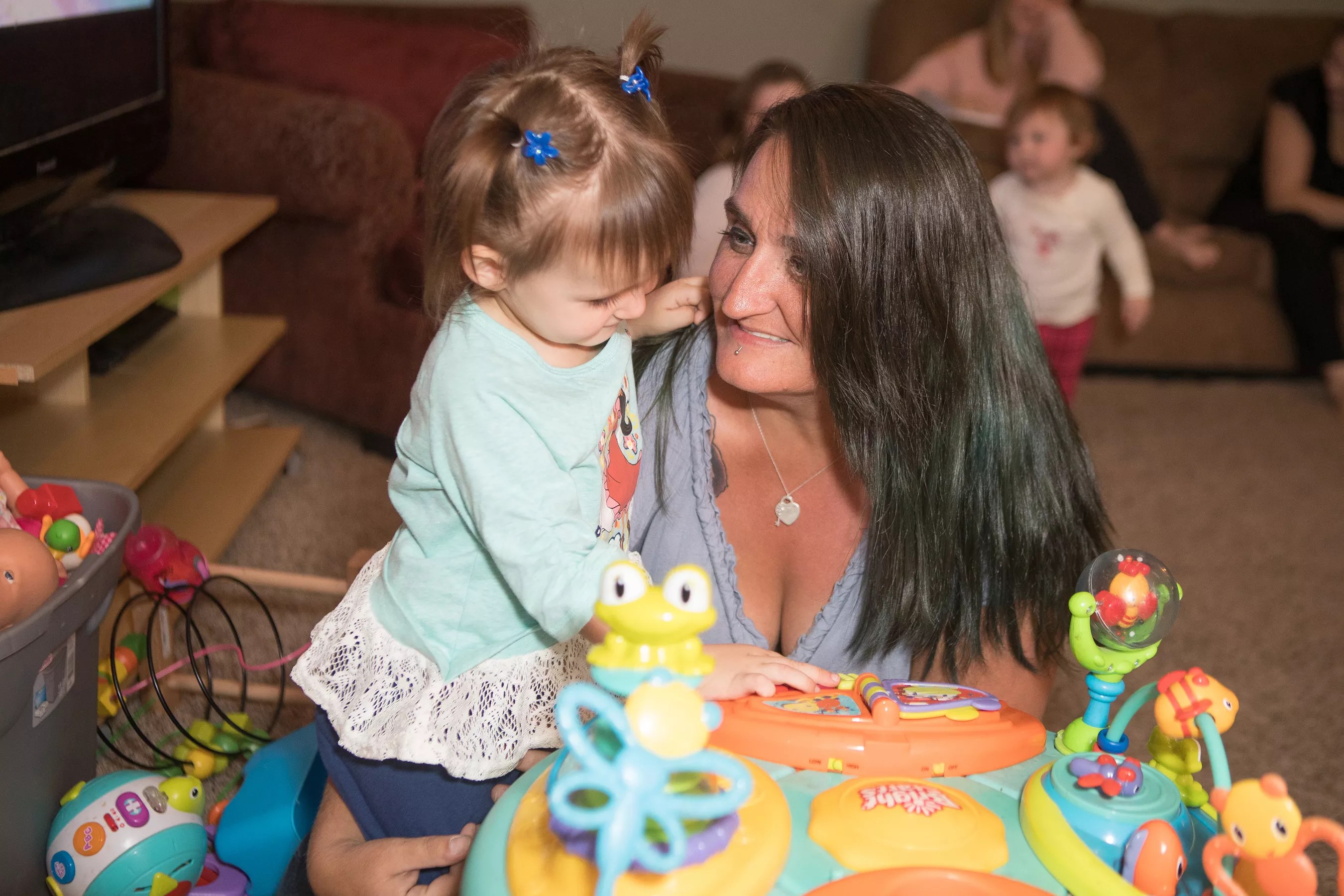
Dorothy Davis lost her job after her daughter
Jim Louvau
There are still goals Emelynn is working to meet.
Her speech is still delayed, but she’s learned sign language for “more,” which she uses often. Sometimes she surprises everyone and blurts out “I love you” or “Where is Dada?”
Dorothy no longer settles for just 80 percent.
She talks about Emelynn going to college one day. The same Emelynn who doctors predicted wouldn’t live much past 30 when they first met her in June.
“Now, with all the progress she’s made, I feel that some day she’s going to tell somebody and they’re going to go ‘I would have never known,’” Dorothy said.
Emelynn can participate in family dinner now, eating solid food after two and a half months on a feeding tube. Even so, most of her food ends up spilling down the highchair and onto the floor for their Catahoula Cur, Bandit, to lap up.
On this day, Russell was grilling chicken outside and Dorothy joined him for a smoke break. She pulled two lawn chairs away from a black iron fence that now surrounds the pool.
Russell, a professional welder, built the fence after the accident. His company donated the materials and other labor free of charge — something it plans to do every summer now for families who can’t afford pool fences.
Dorothy lit her Marlboro. She intended on quitting over the summer. She even bought Chantix pills. But then everything snowballed after Emelynn’s accident and Dorothy lost her job after spending too much time at doctors’ appointments. The financial stress mounted so they rented out a room in their house to help pay the bills.
It wasn’t exactly an ideal time for Dorothy to quit her one vice.
Russell sat down next to her and lit his own cigarette. He is more soft-spoken, less outgoing than Dorothy — they ying and yang. Dorothy teases that without her he wouldn’t speak to a single soul before his third beer.
Russell is more hesitant to talk about Emelynn’s drowning, which the whole family only refers to as her accident. It’s hard for him to accept that 20 adults were in the backyard and yet no one saw Emelynn go under.
Cutting through all the confusion, frustration, and guilt is that nagging question — what the hell happened?
Everyone who was there that day is healing together. Some of The New Founders of Freedom members have sought counseling.
Katelin Steinke, one of the two friends who administered CPR, has decided to go back to school to become a nurse. She got a tattoo of a pink and purple tank on her foot to represent Emelynn, Little Tank.
Brian Christian, the other friend who assisted in CPR, dedicated a poem titled “My Breath” to Emelynn. He wrote, “The light in your eyes has since returned / the sights of that day will forever be burned.”
Dorothy and Russell’s preferred method of therapy is long rides on their Harleys. Russell has a black Heritage Classic with handlebars that come up to his shoulders. He said it looks like death. Dorothy rides a Dyna Low Rider nicknamed Ruby for its red finish.
Still, there’s no amount of open road that can erase that day.
“I’m not 100 percent the same person I was before,” Dorothy said. “I’m trying to be.”
She paused.
“As she gets better, I get better.”

More than six months after her accident, Emelynn is back home in Buckeye.
Jim Louvau
Dorothy described herself as a building that was left standing after an earthquake rolled through.
“I’m holding it together,” she said. “I’m not coming crashing down, but a part of me is still definitively broken.”
Russell put it more simply: “We’re all fucked up about it.”
Emelynn came outside to check on her parents. Dressed in ladybug wings, she was wobbly on the cobblestone patio as she immediately reached for Dorothy. She was getting cranky.
“Hi, crabcakes,” Dorothy said. “Are you getting tired? Let’s get some dinner.”
Emelynn slid down her mom’s leg and explored the backyard. She climbed onto the folding chair Russell had left empty as he checked the grill. Emelynn slid through the back of the chair and landed on the ground, almost bonking her head on the stone.
Dorothy scooped her up and wiped away her tears.
“I got you. I got you.”
This time, Mom was there to protect her.